This one is a little different.
I don’t usually write about politics. That’s not what this practice is about, and it’s not what most of my clients come to me for. But I’d be doing a disservice if I didn’t name something that I’m seeing consistently right now in the women I work with in Washington DC.
The stress here is different lately. And it’s having real physiological effects.
What’s Actually Happening in Your Body
Stress is not just a feeling. It’s a cascade of biological events.
When your brain perceives a threat- whether that’s a deadline, a difficult conversation, or the ambient uncertainty of living in a city where the political ground is constantly shifting- your hypothalamic-pituitary-adrenal (HPA) axis activates. Cortisol and adrenaline are released. Your body prepares to respond.
This is adaptive. In the short term, it’s protective.
The problem is when it doesn’t turn off.
Chronic stress- the kind that runs in the background for weeks, months, or years, has measurable effects on nearly every system in the body. A 2024 review published in Frontiers in Immunology found that chronic stress disrupts immune regulation, promotes systemic inflammation, and directly alters the gut microbiome. 1 A 2025 study in the Journal of Applied Physiology found that prolonged cortisol exposure dysregulates immune function in ways that resemble chronic inflammatory disease. 2
And a 2024 report from the American Psychological Association found that the political climate, economic uncertainty, and the future of the country ranked among the top stressors for Americans- with DC residents living at the epicenter of all of it. 3
The Hormone Connection
For women in perimenopause — which can begin in the mid-to-late 30s — chronic stress doesn’t just add to the burden. It accelerates it.
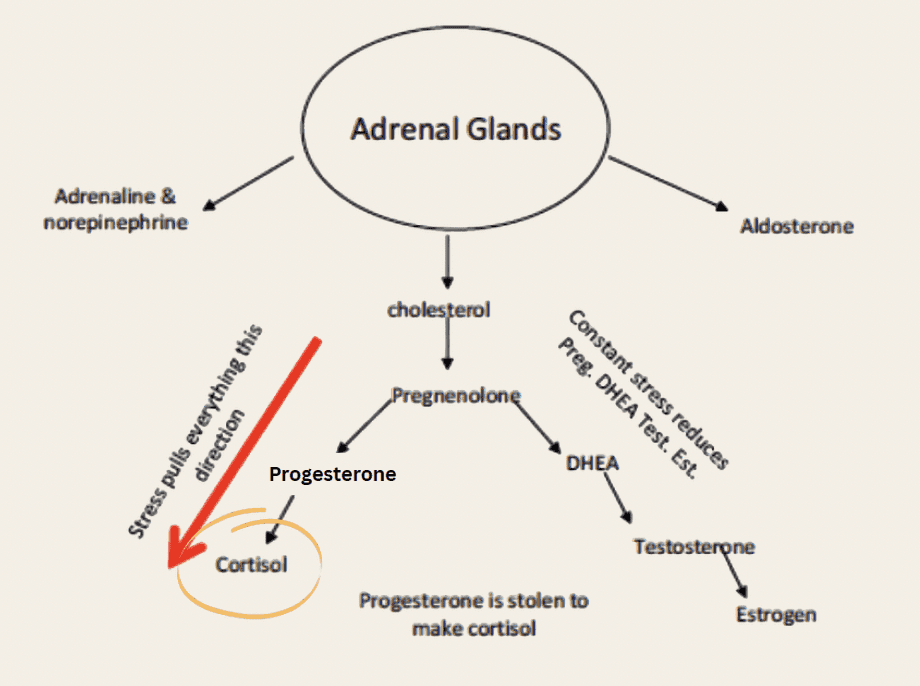
Here’s the mechanism: cortisol and progesterone share a common precursor (pregnenolone). When the body is under chronic stress and cortisol demand is high, it preferentially produces cortisol at the expense of progesterone. This is sometimes called “pregnenolone steal,” and while the term is debated in the literature, the downstream effect — lower progesterone relative to estrogen — is well-documented. 4
Low progesterone in the context of perimenopause contributes to:
•Sleep disruption (progesterone has a calming, sleep-promoting effect)
•Anxiety and irritability
•Heavy or irregular periods
•Breast tenderness
•Worsening PMS
If you’re a woman in your late 30s or 40s in DC who has noticed that your sleep has gotten worse, your anxiety has increased, or your cycles have changed over the past year or two — this is worth paying attention to. It may not be entirely about your hormones. Your stress load is part of the picture.
The Gut Takes the Hit Too
The gut-brain axis is a bidirectional communication system. What happens in your nervous system affects your gut, and what happens in your gut affects your brain and mood.
Chronic stress has been shown to increase intestinal permeability (sometimes called “leaky gut”), alter the composition of the gut microbiome, and reduce the diversity of beneficial bacteria. 5 A 2018 study published in the Proceedings of the National Academy of Sciences found that chronic stress directly disturbed gut microbiota and triggered immune system responses in the gut. 6
This is why so many people in high-stress environments develop digestive symptoms that seem to come out of nowhere — bloating, constipation, diarrhea, food sensitivities that weren’t there before. The gut is responding to the stress load, even when the stress feels “manageable.”
Why This Matters More for DC Residents
I work with clients across multiple states, but DC has a particular character. The people here are often:
•Working in high-stakes environments where performance is expected regardless of how they feel
•Carrying a sense of responsibility that makes it hard to step back, even when the body is asking for it
•Surrounded by others who are also running hard, which normalizes a level of depletion that isn’t actually normal
•Exposed to a news and information environment that keeps the nervous system in a low-grade state of alert
None of this is a character flaw. It’s the environment. But the body doesn’t distinguish between a geopolitical threat and a personal one. It responds to perceived stress the same way.
The question isn’t whether DC is stressful right now. It clearly is. The question is whether you’re giving your body the support it needs to metabolize that stress — or whether you’re accumulating a physiological debt that will eventually come due.
What Functional Medicine Offers in This Context
Functional medicine is well-suited to the kind of complex, multi-system dysregulation that chronic stress produces. Rather than treating each symptom in isolation, it looks at the full picture: hormones, gut, immune function, sleep, inflammation, and the nervous system.
For someone dealing with the effects of chronic stress, this might include:
Adrenal and cortisol assessment. A four-point salivary or urinary cortisol test maps your cortisol rhythm throughout the day — not just a single morning value. This tells us whether you’re in a state of cortisol excess, cortisol depletion (burnout), or a disrupted pattern that’s affecting your sleep and energy.
Comprehensive hormone evaluation. To understand whether stress is affecting your sex hormone balance, and whether hormone support is appropriate.
Gut health assessment. To identify whether chronic stress has disrupted your microbiome or compromised your intestinal barrier — and to address it directly rather than waiting for it to become a bigger problem.
Targeted support. This might include adaptogenic herbs with evidence for HPA axis regulation (ashwagandha, rhodiola), targeted nutrient support (magnesium, B vitamins, vitamin C — all depleted by chronic stress), dietary adjustments, and sleep optimization.
This isn’t about adding more things to your to-do list. It’s about understanding what your body actually needs right now — and addressing it efficiently.
A Note on Timing
I want to be direct about something: the best time to address this is before you hit a wall.
Burnout, adrenal fatigue, and hormonal dysregulation don’t announce themselves with a clear warning. They build gradually, and then they become harder to reverse. The women who do the best in this work are the ones who come in while they’re still functioning well — and want to stay that way — rather than after they’ve already crashed.
If you’re in DC, you’re operating in one of the most demanding environments in the country right now. That’s not going to change anytime soon. What you can control is how well your body is resourced to handle it.
If you want to understand how chronic stress may be affecting your hormones, gut, and overall function — and what to do about it — the first step is a Wellness Evaluation. We’ll take a clear look at where you are and what support makes sense.
About the Author: Ashley is a Doctorate-Prepared Nurse Practitioner and IFMCP-certified functional medicine provider with 10 years of experience working with perimenopausal women and athletes. She practices via telehealth and is licensed in DC, MD, VA, OR, FL, ID, CO, and MA.
References
Footnotes
1. Warren A, et al. “Dangers of the chronic stress response in the context of the gut microbiome and immune system.” Frontiers in Immunology. 2024. https://www.frontiersin.org/journals/immunology/articles/10.3389/fimmu.2024.1365871/full ↩
2. Marwaha K, et al. “Exploring the complex relationship between psychosocial stress and the gut microbiome: implications for inflammation and immune modulation.” Journal of Applied Physiology. 2025. https://journals.physiology.org/doi/abs/10.1152/japplphysiol.00652.2024 ↩
3. American Psychological Association. “Stress in America 2024: A nation in political turmoil.” apa.org. https://www.apa.org/pubs/reports/stress-in-america/2024 ↩
4. Chrousos GP. “Stress and disorders of the stress system.” Nature Reviews Endocrinology. 2009. https://www.nature.com/articles/nrendo.2009.106 ↩
5. Jia H, et al. “Chronic stress, gut microbiota, and immunity: interconnections and implications for health.” Molecular and Cellular Biochemistry. 2025. https://link.springer.com/article/10.1007/s11010-025-05376-y ↩
6. Gao X, et al. “Chronic stress promotes colitis by disturbing the gut microbiota and triggering immune system response.” Proceedings of the National Academy of Sciences. 2018. https://www.pnas.org/doi/abs/10.1073/pnas.1720696115 ↩




Comments +