If you’ve been dealing with bloating, irregular digestion, fatigue, or symptoms that seem unrelated but keep showing up together, there’s a good chance no one has looked closely at your gut.
Not really looked.
A standard stool culture — the kind your gastroenterologist might order — checks for a narrow list of bacterial pathogens. It’s designed to rule out acute infection. It’s not designed to understand the complex ecosystem of your gut microbiome, identify low-grade dysbiosis, or assess whether your intestinal lining is intact.
That’s where the GI-MAP comes in.
What the GI-MAP Actually Measures
The GI-MAP (Gastrointestinal Microbial Assay Plus) is a comprehensive stool test that uses quantitative PCR (polymerase chain reaction) technology — the same DNA-detection method used in COVID testing — to identify and quantify microorganisms in your gut. 1
Unlike a standard stool culture, which relies on growing bacteria in a lab (and only detects what can be grown), the GI-MAP detects the DNA of organisms directly. This means it can identify things that a conventional culture would miss entirely.
Here’s what the GI-MAP assesses:
| Category | What’s Measured |
| Pathogens | H. pylori, C. difficile, parasites, viruses, worms |
| Commensal bacteria | Beneficial species like Lactobacillus and Bifidobacterium |
| Dysbiotic bacteria | Opportunistic organisms that overgrow when the gut is disrupted |
| Fungi/yeast | Candida and other fungal species |
| Intestinal health markers | Zonulin (intestinal permeability), calprotectin (inflammation), secretory IgA (immune function) |
| Digestive function | Pancreatic elastase (enzyme output), steatocrit (fat absorption) |
That last category is important. The GI-MAP doesn’t just tell you what’s living in your gut — it tells you how your gut is functioning. That’s a different question, and it’s one that standard testing doesn’t answer.
Why Your Conventional Doctor Probably Hasn’t Ordered It
This is a fair question, and the answer isn’t that conventional doctors are withholding something from you.
The GI-MAP is a specialty lab test, run through companies like Diagnostic Solutions Laboratory or Genova Diagnostics. It’s not part of standard medical training, it’s not covered by most insurance plans, and it’s not part of the conventional diagnostic algorithm for most GI complaints.
Conventional gastroenterology tends to work through a different framework: rule out structural disease (colonoscopy, endoscopy), rule out acute infection (standard stool culture), and if nothing is found, diagnose a functional disorder like IBS. Treatment then typically focuses on symptom management — fiber, antispasmodics, low-FODMAP diet, or antidepressants for gut-brain symptoms.
This approach works for some people. But it leaves a significant gap for those whose symptoms are driven by dysbiosis, low-grade infection, intestinal permeability, or impaired digestive function — none of which show up on a colonoscopy.
A 2020 study published in BMC Infectious Diseases validated the GI-MAP’s performance for detecting known bacterial and parasitic pathogens in stool samples, finding strong sensitivity and specificity compared to reference methods. 2
What Gut Dysfunction Actually Looks Like
Gut dysfunction rarely looks like just a gut problem. This is one of the things that surprises people most.
When the gut microbiome is disrupted, the effects ripple outward:
Hormones. The estrobolome — a subset of gut bacteria — regulates estrogen metabolism. When it’s disrupted, estrogen can recirculate at higher levels or be cleared too quickly, contributing to symptoms like heavy periods, PMS, mood changes, and breast tenderness. 3
Brain. The gut-brain axis is a bidirectional communication system. Gut dysbiosis is associated with anxiety, depression, and cognitive changes — not because the symptoms are “in your head,” but because the gut produces neurotransmitters (including roughly 90% of the body’s serotonin) and communicates directly with the brain via the vagus nerve. 4
Immune function. Approximately 70% of the immune system is housed in the gut. Chronic dysbiosis and intestinal permeability are associated with systemic inflammation, autoimmune conditions, and poor immune regulation. 5
Energy. Impaired digestion and absorption means you may not be extracting the nutrients you need from food — regardless of how well you eat.
This is why I often run a GI-MAP as part of a comprehensive evaluation, even when a client’s primary concern isn’t digestive. The gut is rarely isolated from everything else.
What Happens After the Test
A GI-MAP result is a starting point, not a prescription. The interpretation requires clinical context — your symptoms, history, diet, stress levels, and other lab findings.
When I review a GI-MAP with a client, I’m looking at the full picture:
•Is there an active pathogen that needs to be addressed directly?
•Is there evidence of dysbiosis — an imbalance in the ratio of beneficial to opportunistic bacteria?
•Are there signs of intestinal permeability (elevated zonulin) that might be driving systemic inflammation?
•Is digestive enzyme output adequate?
•What does the immune marker (secretory IgA) tell us about gut immune function?
From there, we build a targeted protocol. This might include dietary changes, specific probiotic strains, antimicrobial herbs or medications, gut-lining support, or digestive enzyme support — depending on what the data shows.
The goal is not to treat the test. It’s to use the test to understand what your gut actually needs.
Here is an example of my Genova test completed in 2021:
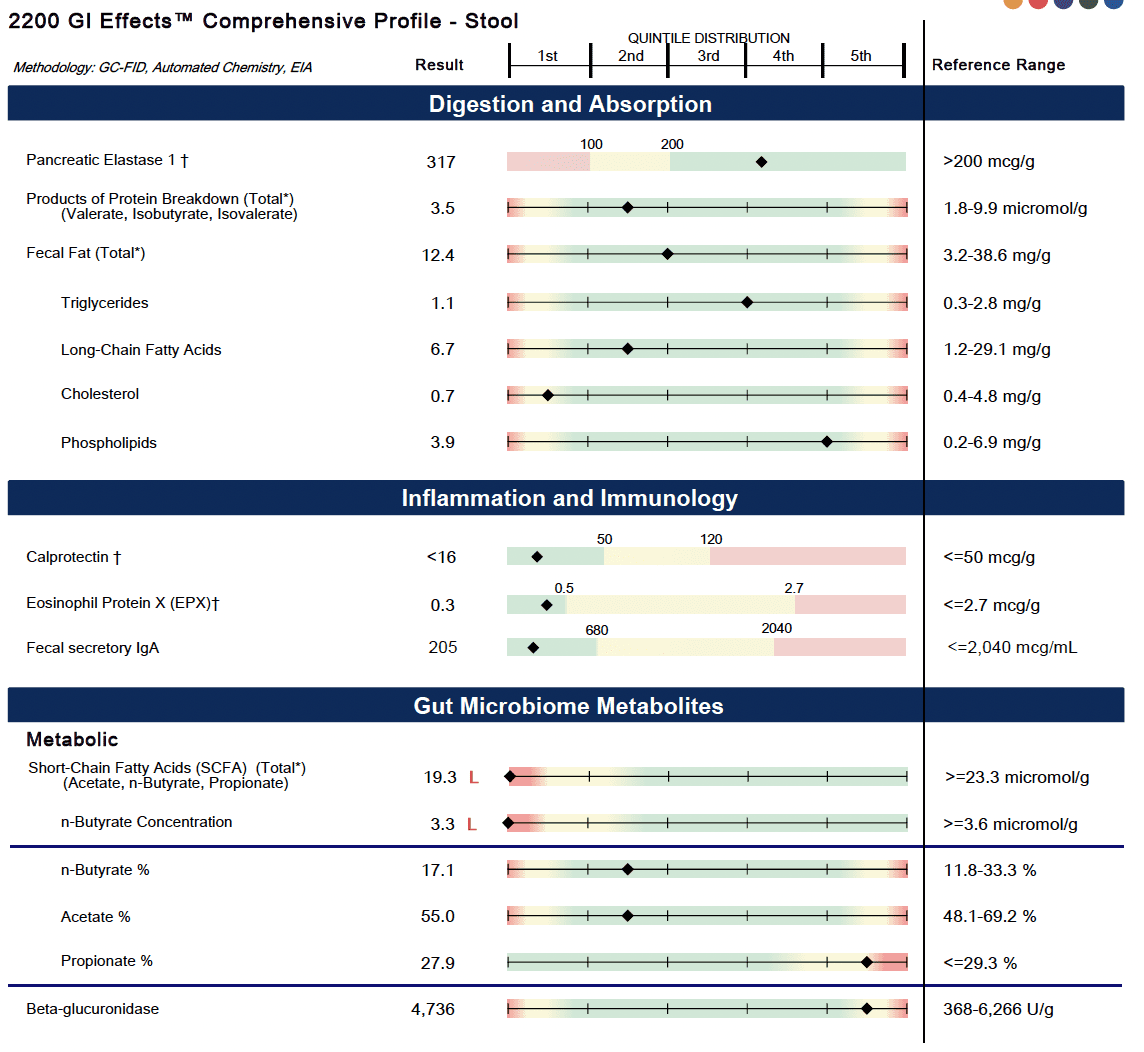
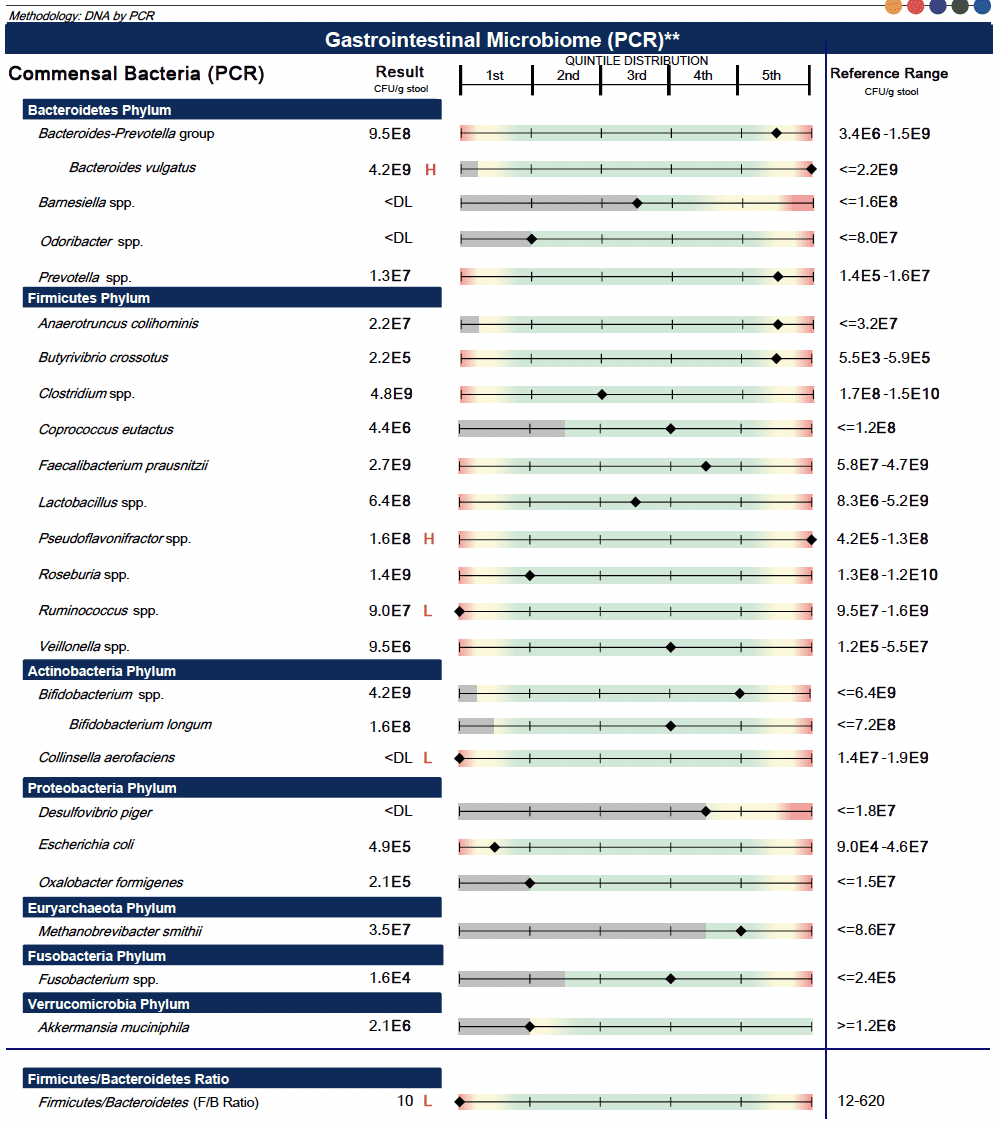
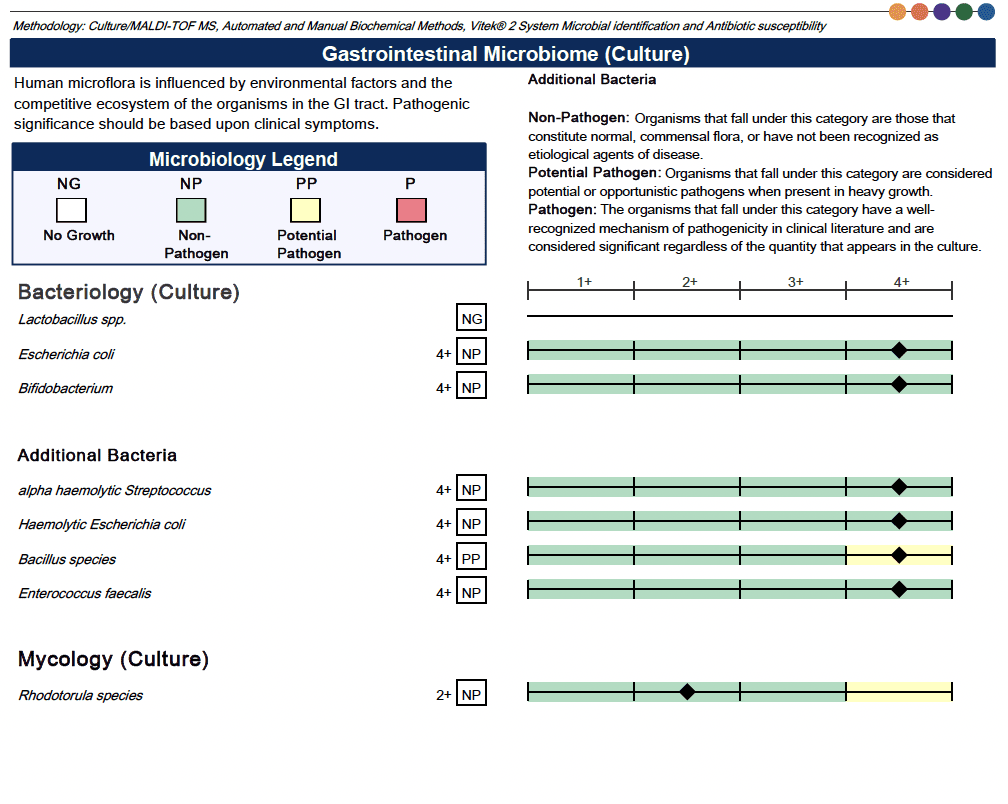
Is the GI-MAP Right for You?
The GI-MAP tends to be most useful if you’re dealing with:
•Chronic bloating, gas, or irregular bowel habits
•IBS diagnosis without a clear cause or effective treatment
•Fatigue and brain fog alongside digestive symptoms
•Hormone imbalance (especially estrogen-dominant symptoms)
•Autoimmune conditions or chronic inflammation
•History of frequent antibiotic use
•Recurrent yeast infections or SIBO
It’s not a test everyone needs. But for the right person, it can be the piece that finally makes everything else make sense.
If you’re in the Washington DC area and want to understand what’s happening in your gut — and how it might be connected to everything else you’re experiencing — the first step is a Wellness Evaluation. We’ll figure out together whether comprehensive stool testing makes sense for you.
About the Author: Ashley is a Doctorate-Prepared Nurse Practitioner and IFMCP-certified functional medicine provider with 10 years of experience working with perimenopausal women and athletes. She practices via telehealth and is licensed in DC, MD, VA, OR, FL, ID, CO, and MA.
References
1.Diagnostic Solutions Laboratory. “GI-MAP: GI Microbial Assay Plus.” diagnosticsolutionslab.com. https://www.diagnosticsolutionslab.com/tests/gi-map ↩
2.Gingras BA, et al. “Performance of a new molecular assay for the detection of gastrointestinal pathogens.” BMC Infectious Diseases. 2020. https://pmc.ncbi.nlm.nih.gov/articles/PMC7660239/ ↩
3.Plottel CS, Blaser MJ. “Microbiome and the estrobolome.” mBio. 2011. https://journals.asm.org/doi/10.1128/mbio.00204-11 ↩
4.Cryan JF, et al. “The Microbiota-Gut-Brain Axis.” Physiological Reviews. 2019. https://journals.physiology.org/doi/full/10.1152/physrev.00018.2018 ↩
5.Vighi G, et al. “Allergy and the gastrointestinal system.” Clinical & Experimental Immunology. 2008. https://pmc.ncbi.nlm.nih.gov/articles/PMC2515351/ ↩




Comments +